|
Audio
Photos
More from MPR
Resources
Your Voice
|
Obesity as a disease
April 11, 2004
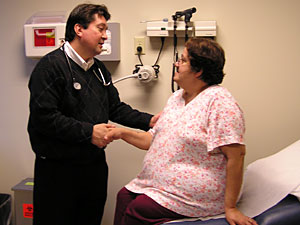 |
| Dr. Michael Gonzalez-Campoy examines Olga, a patient at his new clinic, The Minnesota Center for Obesity, Metabolism and Endocrinology. It's one of the first medical clinics in Minnesota devoted solely to tackling the obesity epidemic. (MPR Photo/Lorna Benson) |
Like smoking, obesity is hard to tackle. Doctors don't have a lot of treatments for patients. There are a handful of marginally effective medications, or in extreme cases, there's gastric bypass surgery to reduce the size of a patient's stomach. But one Minnesota doctor isn't ready to give up. He's staking his reputation on the belief that obesity can be treated effectively if it's treated as a disease.
Eagan, Minn. — Dr. Michael Gonzalez-Campoy is a highly regarded physician. He's president-elect of the Minnesota Medical Association, and serves on Gov. Pawlenty's Task Force on Health Care Disparities. And he heads up the Minnesota Department of Health's Diabetes Plan for 2010.
Despite his credentials, when Gonzalez-Campoy tells his physician colleagues they can help obese patients lose weight, most don't buy it.
"The overwhelming attitude is, 'Why bother? You know, we're not going to be successful anyway, so why try?'" Gonzalez-Campoy says.
His colleagues' skepticism seems to be backed up by statistics. Since the late 1980s, obesity has been climbing steadily in the U.S., even though consumers have spent millions on diet aids and gym memberships.
 | |||
Today about 64 percent of Americans are overweight, and more than 30 percent are obese. It's a staggering problem for physicians to tackle. But Gonzalez-Campoy says they must do something.
"If they ignore obesity, if they don't bring it up, if they don't confront patients with a problem, if they don't deal with a problem, patients are at a disadvantage. And it's time that we as a medical community modify our behavior," says Gonzalez-Campoy.
A recent study published in the Archives of Internal Medicine echos Gonzalez-Campoy's claim. It reports that doctors are failing to take advantage of their authority to influence overweight patients. Researchers say physicians should be measuring waistlines, prescribing exercise drills and preaching healthy eating.
Dr. Gonzalez-Campoy and his staff are doing just that at his new clinic in Eagan -- the Minnesota Center for Obesity, Metabolism and Endocrinology.
On a recent day, one of his patients, Olga, came in for a checkup. Olga is 5 ft. 4 in. tall, and weighs 251 pounds. The 53-year-old St. Paul woman was recently diagnosed with diabetes. Her diagnosis is particularly scary because her mother died from the disease at age 54. Her only brother was even younger when he died from diabetes -- he was 40.
"I'm afraid, sure. I want to do the best I can to try to control it or something, because I got my grandchildren. They need me. Nobody wants to die," says Olga.
For Olga, food has always been an important part of her life, especially sweets. She recalls in vivid detail the memories and flavors from her childhood in Puerto Rico.
|
The only battle we're never going to win is a battle we don't fight.
- Dr. Michael Gonzalez-Campoy |
"Every Saturday in my house, the tradition was to bake a cake Saturday morning. Nobody, my brother, my mother, I myself, we couldn't wait for that cake to get cold. Even warm -- we all had to have it," Olga says, smacking her lips at the memory.
Following her diabetes diagnosis, Olga was referred to Dr. Gonzalez-Campoy. This is her first visit to his clinic. She's here to get help with her diabetes and advice on how to lose weight. But she doesn't want to hear the D-word.
"It's hard to use the word diet. I don't like it. It doesn't motivate me," Olga says.
"I'm delighted to hear that you don't want to diet," says Dr. Gonzalez-Campoy. "I'm going to ask you not to diet. Diet is a four-letter word."
Instead, Gonzalez-Campoy tells Olga to eat more food that's healthy and walk more, even if it's just around the block. He also gives her medicine for her diabetes.
There's medicine for weight loss too. Three drugs have been approved. They have some uncomfortable side effects and most doctors don't prescribe them. But Gonzalez-Campoy thinks they should.
He says most doctors think of obesity as a condition brought on by behavior, so the idea of treating it with medicine is unpopular. He thinks it should be classified as a disease and treated aggressively like other diseases.
"If a patient that's hypertensive walks in and out of an office, they leave with a blood pressure pill. If a patient with obesity comes in, their body mass index is high, and you send them out of the office and you don't treat that obesity -- it would be like sending somebody out with a very high blood pressure and not treating it," he says.
 | |||
But Gonzalez-Campoy isn't just blaming doctors alone for not addressing obesity. He says insurers are a big part of the problem.
"They will not pay for patient care when the diagnosis is obesity. They will not pay for obesity medications. I think that's morally and ethically wrong," says Gonzalez-Campoy. "They're taking money from the patients and the employers to provide care, and they're denying care upfront."
Minnesota's large non-profit insurers pay for some obesity care. But the coverage is spotty. For example, Blue Cross Blue Shield of Minnesota does not pay for any obesity medications. Medica and HealthPartners will pay for one weight loss drug -- Orlistat. But the health plans have strict guidelines, and doctors need to get permission to prescribe it.
Tom Marr works for HealthPartners. He says so far, there isn't much proof that medications or diet and exercise are effective long-term.
"I hate to sound like a broken record, but I come back to what's the evidence that really works in obesity? For example, in the morbidly obese the only therapy that's been shown to be effective, to have long-term impact on the morbidly obese, is weight loss surgery," says Marr. "None of the others -- drugs, diet, counseling -- if you're morbidly obese, has been shown to have long-term positive effect on reducing weight."
HealthPartners has paid for the surgery since 2001. But most overweight and obese patients don't qualify for the procedure because they are not heavy enough.
The gaps in obesity insurance have fueled a debate over whether to call obesity a disease, instead of a condition. Physicians believe the designation would make it harder for health plans to limit treatments. HealthPartners' Tom Marr says the name change isn't necessary because insurers want patients to lose weight, and are trying to find effective ways for them to succeed.
But at the Minnesota Obesity Center, a University of Minnesota research think tank, director Allen Levine says insurers could be do a lot more.
"Certainly you could be cynical about this and say, if somebody's obese they'll die younger and it's going to cost us less. But nobody wants that, and health plans can't be advocating that even if their actuaries tell them that," says Levine.
"It seems to me we have to do something, because right now at the last survey that was done, Mississippi is up to 25 percent of the state being obese, and we're at 65 percent of the public being overweight. It's not going to be long where 100 percent of the public is overweight," Levine says.
Levine thinks Dr. Gonzalez-Campoy's approach is on the right track.
It's a brisk spring day and Olga, Gonzalez-Campoy's new patient, is taking a walk just as he recommended. At first, she struggles. "Yes, today's kind of tough because I wake up very tired. And, you see, I have to stop and breathe and take deep breathing," she says.
But as Olga continue on, she notices how sunny and beautiful it is on the streets of downtown St. Paul.
"You see now I'm out here so I don't mind. Now I don't want to go back," Olga laughs. But she admits it's hard for her to get out the door.
"Yes. Most of the time it's hard. Especially if you have to do it yourself, it's not nice," Olga says.
Dr. Michael Gonzalez-Campoy would agree that it's not easy for patients to lose weight on their own. He says when patients inevitably want to give up, physicians and health plans have to prod them on.
"The only battle we're never going to win is a battle we don't fight," he says.
The Minnesota Center for Obesity, Metabolism and Endocrinology is one of the first medical clinics in Minnesota devoted solely to tackling the obesity epidemic. A handful of other clinics are also beginning to focus on the issue.
|
News Headlines
|
Related Subjects
|

