|
Photos
Resources
|
April 25, 2005
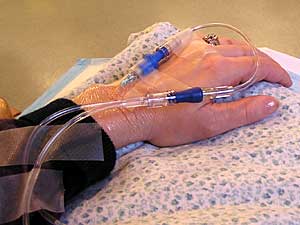 |
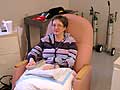
| Remicade is a relatively new drug used for Crohn's disease. It's given through an IV every eight weeks. (Cara Hetland) |
Sioux Falls, S.D. — This story started with a bill, a bill for medication. I'm one of millions of Americans who have to take prescription drugs. Suddenly in January the cost of one of them went up. So I decided to find out why. I have Crohn's disease. It's a chronic infection in my small intestine. The symptoms are unpleasant and there are many things I can't eat. I was first diagnosed ten years ago. I've been on medication since then and I've had one surgery.
Last summer my Crohn's became active I was unable to eat much of anything at all. My doctor, Chris Hurley, decided to put me on the drug Remicade. He says I had two choices.
"In your case in particular, you're on good medication... And when you have recurrence of the Crohn's and problems relating to Crohn's with some evidence of disease activity despite those aggressive measures, the options are to add something like Remicade which we have available now or a surgery which would be the lesser of two choices," says Hurley.
And that's when I started taking the drug Remicade. I receive an infusion every eight weeks through an IV. It takes about two to three hours.
Remicade is what's called a biotech drug. It's one of 160 that have been approved in the past decade. Biotech drugs are derived from living antibody cells. The use of this drug has sky rocketed over the past few years. Remicade is also used for Rheumatoid Arthritis. One Midwestern HMO reports its cost for Remicade went from $300,000 to $2 million over a two-year period.
Remicade is an expensive drug therapy.
In February, I saw the price go up from $3,500 to $4,000 for each infusion. The statement from my clinic had two additional charges. Those indicated that I'd received chemotherapy.
I don't have cancer. So, I called my clinic and they did a billing review. They didn't know why the bill showed a chemotherapy charge. A patient advocate finally told me it was because Remicade was reclassified as a cancer drug. But she couldn't tell me why.
Rosemary Hooten is the pharmacy supervisor at the Sioux Valley Oncology Clinic. She says the additional charge is all about the federal government catching up with safety standards and reimbursement.
Remicade is a toxic drug and the people who handle it have to take protective measures. Hooten says reclassifying Remicade means Medicare will pay for the safety standards the drug requires. She likens it to the left hand knowing what the right hand is doing.
"It's kind of the right hand is concerned with employee safety and patient safety," says Hooten. "So on the one hand, the government is regulating it over here. But on the other side where they're determining what they'll pay for and what they won't pay for and what level they will pay for they don't always jive necessarily," she says.
The federal government can only dictate what Medicare will pay for. My clinic puts the addition charge on my bill for chemotherapy because the federal government allows it. That doesn't mean it's going to get paid.
Medica is my health care insurance provider and Larry Busse is their spokesman. He says what I see on a statement is not what Medica pays to the clinic and he says private insurance does not follow federal Medicare standards.
"We already have a reimbursement agreement for the medications. We can look at the medicare changes and if they made sense we may choose to follow them. We don't have to do that," says Busse. "We probably wouldn't do that if it would result in an increase cost to the medication. Part of our job is to hold costs down."
Ten years ago when I was first diagnosed with Crohn's, Remicade didn't even exist. Dr. Hurley says that's the best therapy for me right now. He says genetic therapy is on the horizon and maybe in my lifetime there will be a cure for Crohn's disease. As new treatments become available and who knows, maybe the cost for Remicade will go down.