July 24, 2005
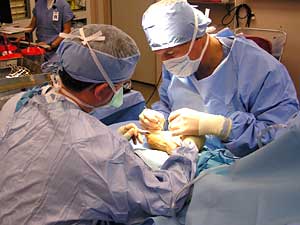 |
| Dr. Mark Holm operates on a patient's hand after verifying that he is performing the correct procedure on the correct person. (MPR Photo/Lorna Benson) |
St. Paul, Minn. — The project clearly has an ambitious and somewhat grandiose name. It's called "Safest in America." But the hospitals say the title accurately represents what they hope to achieve as a result of their collaboration with each other.
Their unusual partnership formed a few years ago in the wake of a disturbing study from the Institute of Medicine. That 1999 report calculated that up to 98,000 patients die in U.S. hospitals each year because of medical errors.
David Page, chair of "Safest in America," says at the time, the findings sent shock waves through hospitals everywhere.
"The reaction was, 'Oh my God. If half of that is true, this is a huge issue,'" Page says. "You just couldn't turn your back and say, 'Oh, that's a bunch of hooey. They did this or that wrong.' Because even if they did it wrong the numbers were so large."
Still, it took two more years before "Safest in America" was born. That's when former HealthPartners CEO George Halvorson personally invited 10 hospital CEOs to a top-secret breakfast meeting.
Halvorson suggested a plan that sounded simple. He wanted hospital leaders to share their data every time an error occurred in their hospital, so everyone else could learn from the mistake.
But the idea wasn't an instant hit. David Page, who's also CEO of Fairview Health Services, was at the meeting.
"I left it thinking, 'Well, good luck. I don't know what will come of this,'" says Page. "I may not have been the only skeptic. But I certainly will admit to my skepticism."
Page says he thought the problem was just too big.
"I was a little concerned that we were maybe coming together in a bit of a naïve fashion," says Page, "to think this problem of this magnitude was going to be something that our collaborative effort would make any real headway on."
Page ultimately decided that it was too big of a problem not to do something about it. And after a few more meetings, all of the hospital CEOs signed on to Halvorson's plan.
As part of the agreement, the hospitals don't release their data publicly unless the state requires it. Allina Vice President Barbara Balik says that stipulation is critical. Because the information is kept confidential, she says the hospitals are more comfortable sharing their mistakes.
"We're reporting things that no one else in the country reports," says Balik, "because we decided to land on the side of reporting more so we could learn from those events."
The hospitals quickly decided that their top priority was eliminating wrong-site surgeries -- procedures where a doctor mistakenly operates on the wrong body part. These errors are rare, but when they happen they're devastating for the patient, the physician, and the hospital.
After studying the problem, the hospitals decided to make a big change in their pre-operative procedures. Page says there was just too much variation from hospital to hospital when it came to marking where to operate on a patient's body.
The differences were especially problematic for doctors and nurses who work at more than one hospital.
"Some of the institutions would mark where you wouldn't go," says Page. "Others were marking where you would do surgery. Wow. Now there's a polar opposite and it would be very confusing."
Page says the hospitals agreed to a new policy that doctors would only mark body parts that required surgery. After a phase-in period, the requirement became mandatory at all "Safest in America" member hospitals in February.
At the same time, the hospitals also launched what they call "Pause for the Cause." It's a last-minute verification just before an operation begins.
On a recent morning, a surgical nurse in an operating room at St. Joseph's Hospital in St. Paul read through the checklist.
"All right, pause for the cause," she began. "Theresa Albright-Fischer is our patient, for left thumb carpal metacarpal anthroplasty, with artalon carpal metacarpal spacer, with Dr. Mark Holm."
Orthopedic surgeon Mark Holm then told his staff he agrees with the procedure, and then he began to work on Albright-Fischer's thumb joint.
As a surgeon, Holm is used to asking questions and verifying information. Even so, some of his hospital's new patient safety policies were a bit of an adjustment for him.
"I have to admit, even in the beginning it seemed kind of silly and very redundant," says Holm. "It wasn't unusual for me to get a page saying, 'Dr. Holm, you forgot to mark the patient's shoulder.' But as time went along I saw the benefits of it, and I think it's a very valuable tool to prevent mistakes."
But have "Pause for the Cause" and surgical site marking guidelines actually reduced errors in the operating room? The short answer is no, at least not according to the numbers.
Gordon Mosser is executive director of the Institute for Clinical Systems Improvement, also known as ICSI. Mosser's organization analyzes the error data submitted by "Safest in America" hospitals.
Among the 17 Minnesota hospitals participating in the project to share surgical data, Mosser says there are about 35 errors per one million procedures. He says that number hasn't changed much in the four years that his organization has been tracking it.
"It's very frustrating," says Mosser. "I think they really have dropped, and that the drop has been balanced by improved reporting."
Mosser says more situations are now being counted as surgical errors -- for example, if the lab sends the wrong chart to the physician and that causes a mistake.
"At one point, these errors due to something wrong with the laboratory wouldn't have been construed as surgical errors," says Mosser. "But I think that is being too easy on ourselves not to count them that way."
Even if the numbers don't support it yet, Mosser says there clearly have been successes associated with the surgical data sharing. He points to one error in particular that resulted in immediate changes across the hospital systems.
Mosser says shortly after "Safest in America" began, a hospital reported that one of its doctors had performed a wrong-site spine surgery on an obese patient. Two other hospitals quickly replied that they had experienced similar situations.
Mosser says the hospitals realized in a matter of minutes that there was a problem with the marking procedure.
"Marking the skin isn't quite good enough, because the relationship of the mark on somebody's skin to the backbone can shift," says Mosser. "So we added X-ray requirements to the procedure in order to decrease those, and we have been able to get rid of those."
"Safest in America" chair David Page says hospitals would prefer to have data that shows a decline in mistakes.
"We very much want to see statistical evidence that the tracks we're making are making a difference. It's not quite so apparent in, say, surgery. We've had other areas where it's very evident," says Page.
Although the project started in the realm of surgery, Page says it has spread to other areas. He says the hospitals have reduced prescription errors by eliminating nine abbreviations that could be misinterpreted by pharmacists. He says they've also made medications safer for kids by dispensing them based on the child's weight, not age.
Many "Safest in America" hospitals report that they have reduced the occurrence of potentially dangerous blood sugar problems with better monitoring.
The "Safest in America" group hopes to create an anthology of the problems they've tackled. They believe it could help other hospitals around the country that want to team up to improve patient safety.