|
Photos
More from MPR
Resources
|
July 14, 2005
University of Minnesota researchers have figured out a way to reverse memory loss in mice with dementia. The discovery could lead to new treatments for Alzheimer's disease in humans. The findings are published in the latest edition of the journal "Science."
Minneapolis, Minn. — In the study, mice were genetically altered to develop a rare form of dementia found in humans. To do that U of M researchers used a special gene, known as a transgene, that contained a mutant form of a common protein called tau.
Tau is one of two proteins widely associated with Alzheimer's disease. The scientists then created a way to turn the defective tau protein on and off using a common antibiotic.
When the mice were a month old, researchers tested their memory capacity for the first time in a water maze. Lead author of the study, Dr. Karen Ashe, says the maze consisted of a small pool with a hidden platform that was submerged about a half a centimeter below the surface.
"Mice are really good swimmers, but they don't like to swim," says Ashe. "So they're motivated to find the platform."
The platform was kept in the same place until the young mice learned where it was located. Then researchers removed it and measured the percentage of time that the mice spent looking for the platform in the correct location in the pool.
"Even though this test seems like a very simple test, it's actually fairly complex for a mouse," says Ashe. "And it tests a part of the brain that really is critical for initiating and consolidating memories."
Since the mice were only a month old, their dementia wasn't noticeable yet and Ashe says they performed well in the maze. She says they spent about 50 percent of their time in the correct quadrant of the pool as they searched for the missing platform.
But as the mice aged and their dementia progressed, their success rate dropped significantly, just as Ashe thought would happen.
That's when researchers decided to shut off the defective tau transgene. Then, they tested the mice again. The findings were much better than expected.
"We were quite surprised with the results of the experiment, because we had expected that we would halt the progression of memory loss," says Ashe. "But we actually restored memory in these mice."
Ashe suspects that memory function returned because the mice hadn't lost any of their neurons yet. They were damaged, but they were all still functioning.
So researchers turned the defective tau gene back on and let the dementia progress further in the mice. When they shut if off again a few months later, Ashe says the animals were still able to recover memory capacity, but they weren't able to learn as much as before. Ashe says that's because by this point in their dementia, some of their neurons had died.
But she thinks the findings should still give Alzheimer's researchers a lot of hope, because it means that memory can possibly be restored in humans too, if Alzheimer's is treated early.
Researchers hope to apply this approach to humans, but Ashe says scientists still don't know for sure which molecules need to be blocked.
"If we can identify them and understand how they form," says Ashe, "then we may be able to develop drugs that prevent those molecules from forming, or develop drugs that help them to be cleared more rapidly from the neurons and from the brain."
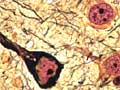
Ashe says her findings also suggest that Alzheimer's research has been too focused on things that are apparently just symptoms of the disease, not its cause, namely plaques that build up in the brain and another feature called neurofibrillary tangles.
Ashe says in her study, those tangles kept growing even as memory function improved in the mice.
"There's such a stark contrast between the accumulation of neurofibrillary tangles and the improvement in memory that makes it obvious that the neurofibrillary tangles could not be the cause of memory loss," she says.
Ashe says the neurofibrillary tangles are clearly caused by Alzheimer's disease, but she says they could be either an innocent bystander or they might be a way to protect the brain from toxins generated by the disease. She says that research is the focus of another paper she's working on.